A practical resilience-and-finance playbook for critical access hospitals, rural clinics, and community care hubs.
This article is a collaborative effort by Shiva Subramanya, Erick Spink, Shane VanCise, and Becky Werra, representing the views of Veregy.

Who this is for
This article is designed for:
1. CEO/CFO/COO/CNO of rural hospitals, critical access hospitals (CAHs), rural emergency hospitals (REHs), and clinics
2. Facilities directors and plant operation leaders managing deferred maintenance and compliance
3. Health system leaders supporting rural affiliates (capital allocation, standards, procurement)
4. Grant and program managers building fundable resilience projects
5. Rural health policymakers focused on access, continuity, and community resilience
Why such a broad audience? Because EaaS is not just an energy project. It’s a care continuity program that spans:
- Clinical risk and emergency planning (Centers for Medicare and Medicaid Services (CMS) Emergency Preparedness Rule expectations) (CMS, n.d.)
- Facilities and life safety (including evolving codes and interpretations that increasingly acknowledge microgrids) (CMS, 2023)
- Finance and contracting (multi-year obligations vs capital constraints)
- IT and cybersecurity (connected controls, monitoring, and interoperability) (National Institute of Standards and Technology [NIST], 2023)
Rural realities matter here. The U.S. Government Accountability Office (GAO) has documented that rural hospital closures reduce access to services and can force patients to travel farther for care, making continuity and resilience not just operational issues but access issues. At the same time, rural hospitals face intensified financial pressure; recent analyses from The Chartis Center for Rural Health describe a growing share operating in the red. (U.S. Government Accountability Office [GAO], 2020; Chartis Center for Rural Health, 2024) (Even if your facility is stable today, your community’s resilience depends on your ability to stay open tomorrow.) More recently, reimbursement changes in Medicare and Medicaid can tighten margins and borrowing capacity, reducing capital appetite and pushing leaders to prioritize solutions that improve resilience without large upfront spend.
Top Benefits Of EaaS For Rural Healthcare
EaaS can be structured in many ways, but the best programs consistently deliver five outcomes, that combine reliability, infrastructure modernization and cost control with sustainability, not sustainability alone:
- Resilience you can measure
- Defined critical load coverage (kW) and ride-through time (hours/days) (the amount of time your facility can keep critical services running without interruption)
- Clear uptime targets and response commitments, aligned with emergency preparedness guidance, according to the Federal Emergency Management Agency. (FEMA, 2020)
- Capital avoidance without standing still
- Upgrades proceed without waiting for scarce capex cycles
- Payments tied to performance, availability, or verified savings (structure matters)
- Operational lift for lean teams
- Remote monitoring, preventive maintenance, and 24/7 support
- A reliable, repeatable program; not a “fire drill” every time something breaks.
- Lower energy waste and better cost predictability
- Many hospitals have wide performance variation (ENERGY STAR), indicating practical savings potential (EPA, 2015)
- EaaS can bundle efficiency and controls (often the quickest ROI) with resilience assets
- Cleaner backup strategy and improved community health
- Diesel exhaust has well-documented health impacts; reducing runtime and right-sizing backup can be meaningful for patients and staff (EPA, n.d.-a)
EaaS Basics
Energy as a Service (EaaS) is a contract model in which an energy partner designs, finances (through a financial partner), installs, operates, and maintains a set of energy improvements,
and you pay for the service over time, typically tied to agreed-upon performance outcomes (savings, availability, or both).
The American Council for an Energy-Efficient Economy (ACEEE) describes service-based models in which customers repay through periodic fees tied directly or indirectly to realized savings, often with the provider taking on performance risk. (ACEEE, 2019)
Many EaaS deals resemble a family of “as-a-service” structures:
-
- Energy Service Agreements (ESAs) for efficiency (provider may own equipment during term) (DOE, n.d.-a)
- Power Purchase Agreements (PPAs) for onsite generation (pay per kWh)
- Availability/resilience contracts (pay to keep backup power ready and reliable), so your critical services can keep running during an outage. You are not paying for the electricity you use. You are paying for readiness and performance.
In practice, rural healthcare often benefits from bundling: efficiency, controls, backup modernization, onsite generation, storage, microgrid controls, and operations and maintenance (O&M).
How This Differs From Traditional EPC/ESPC
Energy Savings Performance Contracting (ESPC) typically guarantees energy savings, with financing arranged (through a financing partner) so the savings help pay for improvements. The Environmental Protection Agency’s (EPA’s) overview of performance contracting and ESPCs highlights that ESCOs implement projects and guarantee savings levels. (EPA, n.d.-b)
EaaS overlaps with EPC/ESPC but often expands the scope to include ongoing operational responsibility and asset ownership/operation during the term, especially when distributed energy resources (DER) and controls are involved.
History Of EaaS
Energy systems were once treated as a simple commodity: buy electricity (and fuel), own the equipment, and rely on internal teams to keep everything running. As regulations, performance expectations, and technology have evolved, energy is no longer just a bill to manage; it’s an operational system that affects clinical continuity, safety, and budgets. (Iconic Bule, 2023) EaaS brings these pieces together by shifting from “owning and maintaining infrastructure” to “contracting for outcomes,” such as predictable costs, verified efficiency improvements, and reliable power for critical loads like Emergency Department (ED) operations, refrigeration, and IT/telehealth. In practice, it enables rural hospitals and clinics, often facing limited capital and lean facilities staffing, to modernize aging systems with performance guarantees and ongoing operational support, rather than waiting for the next scarce capital cycle.
Why Energy Is A Clinical And Financial Issue In Rural Care
Rural healthcare leaders already manage the “known hard things”: thin margins, recruitment challenges, payer mix volatility, and aging buildings. What’s changed is that energy reliability and energy cost volatility are now colliding with care delivery in ways that show up in clinical risk, operational capacity, and financial performance.
Even routine outages can become clinical events when they disrupt any of the following:
- ED and inpatient care (lighting, medical air, suction, imaging)
- Operating Room (OR)/procedures (sterile HVAC, power quality, uptime)
- Vaccine and medication refrigeration
- Water, sanitation, and infection control systems
- Heating/cooling during extreme temperatures (patient safety, sheltering)
According to the U.S. Energy Information Administration, reliability metrics such as the System Average Interruption Duration Index (SAIDI) and the System Average Interruption Index (SAIFI) explicitly separate “major event days” from normal operations, as extreme weather is increasingly the driver of long outages. (EIA, 2023) For rural sites at the end of long distribution feeders, restoration can be slower simply because there’s more line per customer to repair.
Meanwhile, hospitals are energy-intensive buildings. ENERGY STAR benchmarking shows the hospital energy use intensity varies widely (from <100 to >1,400 kBtu/ft2 across hospitals), meaning many facilities have both high exposure and real efficiency headroom. (EPA, 2015). DOE’s Better Buildings program notes that healthcare uses a disproportionate share of commercial energy, reinforcing why energy strategy is now part of core operations. (DOE, n.d.-b).
Energy as a Service is one of the most practical tools for responding, especially for rural organizations with limited capital and bandwidth. Done well, EaaS can convert a complicated bundle of upgrades (efficiency + onsite power + controls + maintenance) into a performance-backed service with predictable payments.
Exhibit A: Clinical risk often begins with non-obvious loads, such as HVAC, IT, and refrigeration. Energy planning isn’t just “keeping the lights on”; it’s protecting care pathways. If energy fails, care pathways fail, so energy strategy belongs on the same dashboard as quality, finance, and emergency preparedness. (FEMA, 2020)

Rural healthcare is uniquely impacted
The rural grid and the rural facility are both “long-tail” (rare, high-impact events) problems. Rural outages are not only about frequency; they’re about restoration time and resource constraints. The U.S. Energy Information Administration (EIA) tracks reliability using SAIDI and SAIFI, and it distinguishes major-event days because the most severe impacts tend to be concentrated in disruptive events. (EIA, n.d.) EIA reported the average customer experienced about 5.5 hours of interruptions in 2022 (including major events). (EIA, 2023)
For rural hospitals and clinics, the operational consequences are amplified by:
- Fewer backup redundancies
- Older electrical infrastructure and deferred maintenance
- Limited onsite engineering coverage
- Supply chain fragility during regional disasters (fuel delivery, parts, contractor availability)
Emergency preparedness isn’t optional
The Centers for Medicare & Medicaid Services (CMS) Emergency Preparedness Rule establishes requirements for planning, policies, communication, and training across provider types. (CMS, n.d.) When facilities rely on generators for compliance, CMS-related guidance emphasizes meeting operational needs (including HVAC capability where required). (ASPR, 2019)
The U.S. Department of Health and Human Services (HHS), Assistant Secretary for Preparedness and Response (ASPR), Technical Resources, Assistance Center, and Information Exchange (TRACIE) and Federal Emergency Management Agency (FEMA) both provide healthcare-specific guidance for power outages, highlighting the need to identify critical systems, plan for fuel and staffing, and coordinate with community partners. (ASPR, n.d.; FEMA, 2020)
Diesel dependence has real tradeoffs
Diesel generators are familiar and often necessary, but they can fail, require rigorous testing and maintenance, and create local air quality impacts. EPA notes that exposure to diesel exhaust poses a risk to human health and supports efforts to reduce diesel emissions. (EPA, n.d.-a)
Outage Duration: Normal Conditions vs Major Events
Rural facilities face a compounding risk: greater disruption impact, fewer internal resources, and more challenging restoration logistics.
Exhibit B: Most pain comes from major events; planning should target long-duration outages. Even if “typical” reliability looks acceptable, your risk is concentrated in a few severe events, exactly when rural logistics are hardest.

Five Outcomes Rural Healthcare Can Demand from EaaS
Exhibit C: EaaS is best understood as contracting for energy outcomes, such as uptime, cost savings, and operational performance, rather than purchasing individual assets. Instead of buying equipment, customers procure a performance-guarantee portfolio that may include generation, storage, controls, and ongoing support.
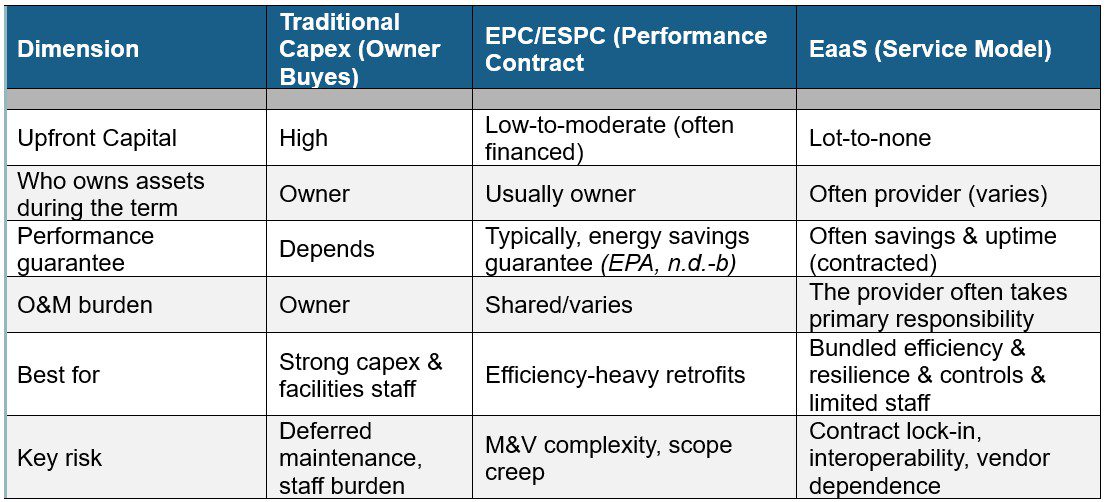
Three pathways to modernize rural healthcare energy systems
The right choice depends on capital constraints, risk tolerance, and internal O&M capacity.
Exhibit D: EaaS shifts more performance and maintenance responsibility to the provider but requires stronger contract discipline. EaaS is not “better” than EPC or capex by default, but it can be uniquely well-suited to rural constraints when structured with clear performance and exit options.
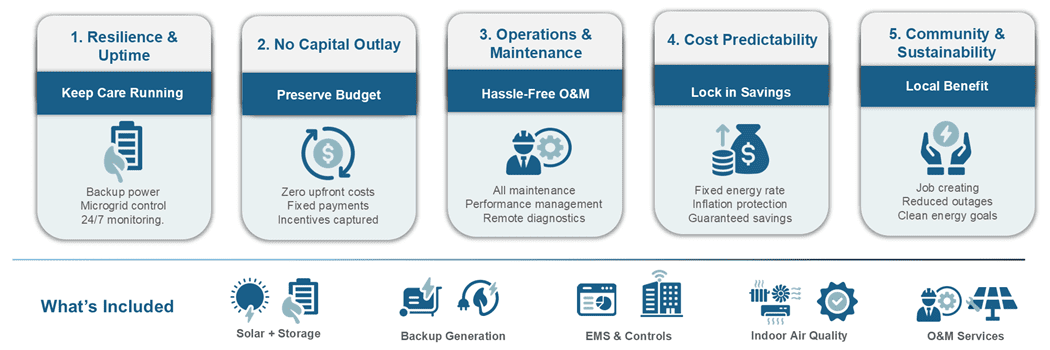
Benefits Of EaaS And What To Demand Contractually
A) Resilience & reliability (continuity of care)
EaaS can contract for resilience outcomes such as:
- Critical load served (kW) during outages
- Ride-through duration (hours/days) with defined assumptions
- Automatic islanding capability (microgrid operation)
- Black start (ability to start your onsite power system when the grid is down) and restoration sequencing
- Power quality for imaging/IT loads
- Testing cadence and reporting
The National Renewable Energy Laboratory (NREL’s) microgrid conceptual design guidance emphasizes a structured process: define loads, assess risk scenarios, model solutions, and validate controls and operations. FEMA’s guide emphasizes improving facility resilience to outages through planning and system design. (NREL, 2019; FEMA, 2020) Also important: CMS survey and code interpretations are increasingly acknowledging microgrid approaches in the healthcare context (e.g., references to healthcare microgrid systems in relation to National Fire Protection Association (NFPA) 99 editions). (CMS, 2023)
B) Financial outcomes (capex avoidance & predictability)
Rural hospitals under financial stress can struggle to justify large capex even when ROI is strong. GAO documents the access consequences of rural hospital closures, while industry analyses highlight operating margin stress. (GAO, 2020; Chartis Center for Rural Health, 2024)
EaaS can help by:
- Shifting capex into a service payment
- Smoothing costs into predictable budgets
- Enabling bundled measures so “fast payback” efficiency helps support resilience assets
C) Operational lift (outsourced O&M, monitoring, guarantees)
With lean teams, outsourced monitoring and maintenance can be as valuable as the equipment.
EaaS often includes:
- 24/7 monitoring and alarms
- Preventive maintenance schedules
- Compliance documentation support (testing logs, performance reports)
- Parts and service response commitments
D) Sustainability & compliance
Efficiency reduces emissions and operating costs simultaneously. DOE Better Buildings reports healthcare partners have saved substantial dollars since 2011 and notes the sector’s outsized energy footprint. (DOE, n.d.-b) Because hospitals use so much energy, even small improvements can materially reduce operating costs, and high baseline demand means you need more backup capacity to sustain critical services during outages.
EaaS can also incorporate cleaner onsite generation, storage, and demand response, while maintaining clinical reliability requirements
E) Patient & community benefits (public health and resilience)
When the hospital stays online, the community retains:
- A place for triage and stabilization
- A warming/cooling center during temperature extremes
- Continuity for dialysis coordination, oxygen-dependent patients, and home health support
The EaaS Stack for Rural Healthcare
A complete performance package combines equipment, controls, contract structure, and ongoing operations.
Exhibit E: EaaS works when the technical and contract stacks match. Controls and O&M are not “extras”; they’re what turns equipment into reliable clinical service. EaaS is most powerful when it bundles efficiency, resilience, and operations into a single accountable performance package. (NREL, 2019)
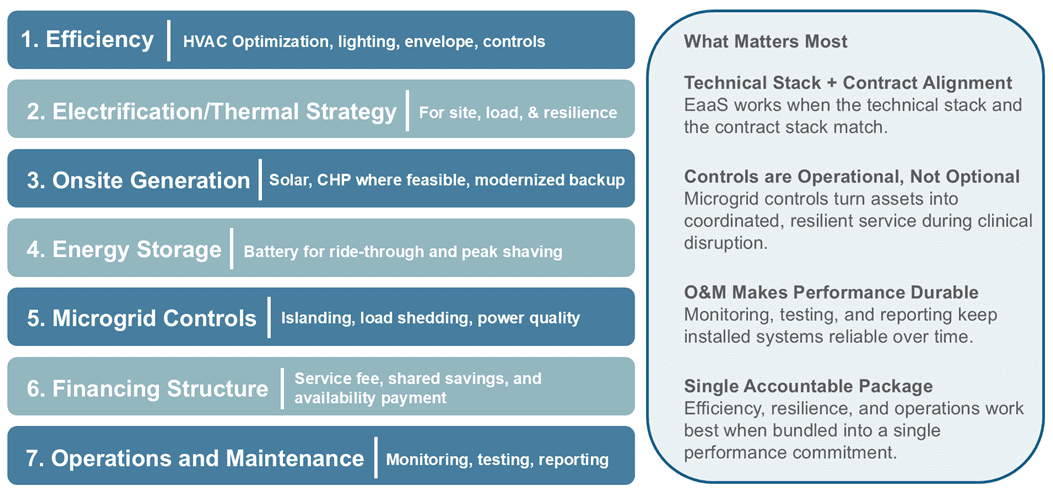
Use Cases And Archetypes
Below are common archetypes with “right-sized” EaaS scopes.
Archetype 1: Critical access hospital (single campus)
Typical pain points: aging switchgear, generator testing burden, HVAC reliability, peak demand charges, and limited capital.
EaaS package idea:
- HVAC controls optimization & recommissioning
- LED & lighting controls
- Battery storage for ride-through & peak shaving
- Solar, where site conditions allow
- Microgrid controller to prioritize ED/OR/MED/refrigeration/IT
- Generator modernization and testing plan
Archetype 2: Rural clinic network (multiple small sites)
Typical pain points: uneven building conditions, small staff, refrigeration issues, and IT vulnerabilities.
EaaS package idea:
- Standardized controls & remote monitoring across sites
- Small storage for refrigeration/IT ride-through
- Efficiency bundles (lighting, heat pumps where feasible)
- Coordinated procurement and reporting
Archetype 3: Long-term care / skilled nursing
Typical pain points: HVAC continuity, resident safety, staffing constraints.
EaaS package idea:
- HVAC resilience (thermal strategy & backup power for key zones)
- Load management & generator coordination
- Indoor air quality and ventilation reliability planning aligned with outage guidance (FEMA, 2020)
Archetype 4: EMS/dispatch & community resilience hub
Typical pain points: communications uptime, fuel logistics, and serving as a public shelter.
EaaS package idea:
- Dedicated critical power & storage
- Hardened telecom & power conditioning
- Islanding plan for multi-day operation
Archetypes and the Critical-Load “Minimum Viable Microgrid”
Start with what must stay on, then build outward.
Exhibit F: The smallest viable resilience package is often storage + controls + targeted circuits, not a full campus rebuild. The best rural EaaS scopes are “clinical load first” and avoid overbuilding.
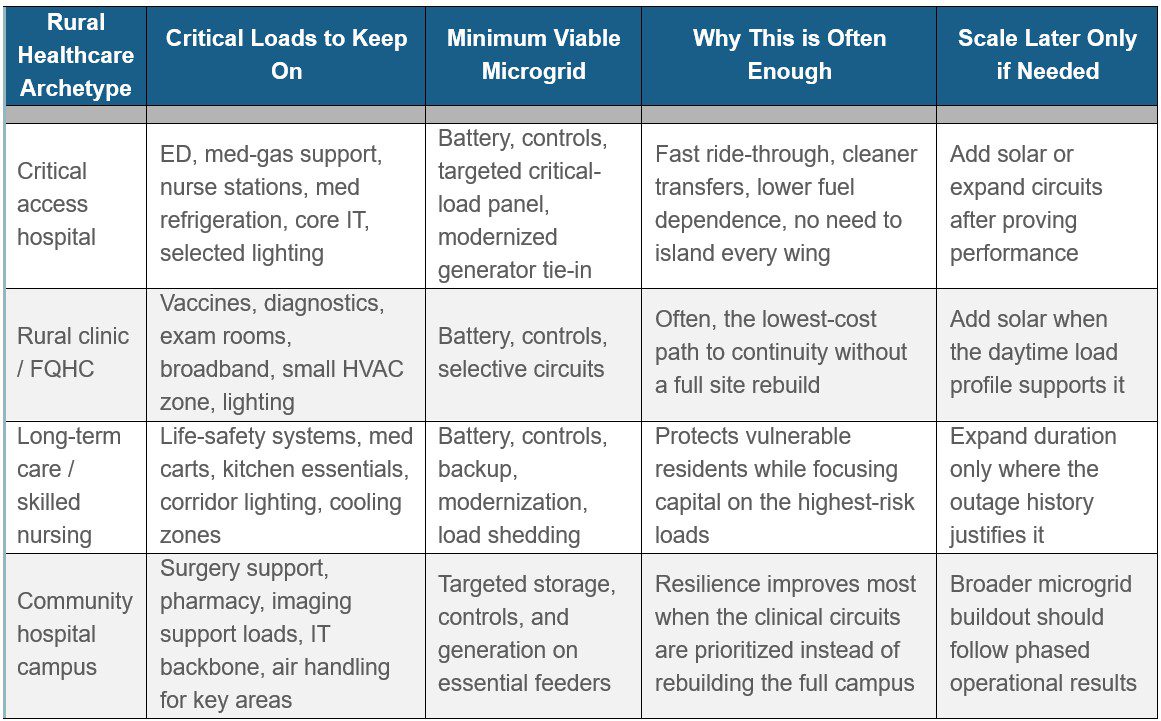
What an EaaS project includes
Think of EaaS measures in four buckets:
Bucket 1: Reduce the load you must back up
- Recommissioning (fixing control sequences)
- HVAC optimization and VFDs
- Lighting retrofits and controls
- Envelope improvements where feasible
The cheapest kWh is the one you never use!
Hospitals show wide variance in energy performance, which is why efficiency is often the first and highest-confidence component. (EPA, 2015)
Bucket 2: Make energy “interruptible without harm”
- Load shedding priorities (clinical vs non-clinical)
- Temperature setbacks for non-occupied zones during outages
- Generator testing integrated with clinical operations
Bucket 3: Add and orchestrate onsite distributed energy resources
- Solar PV (when feasible)
- Battery storage (ride-through + peak + resilience)
- Combined heat and power (CHP) (where there is a strong thermal load and gas reliability)
- Modernized backup generation and switchgear
NREL emphasizes defining resilience objectives and designing accordingly, rather than starting with a favorite technology. (NREL, 2019)
Bucket 4: Controls, monitoring, and cybersecurity
Microgrids and building controls are connected systems. The National Institute of Standards and Technology (NIST) Operational Technology (OT) security guidance explicitly includes building automation systems, which is directly relevant when your energy systems become more software-defined. (NIST, 2023)
Also consider broader sector guidance on DER/distribution cybersecurity baselines as the ecosystem evolves. (DOE, n.d.-c)
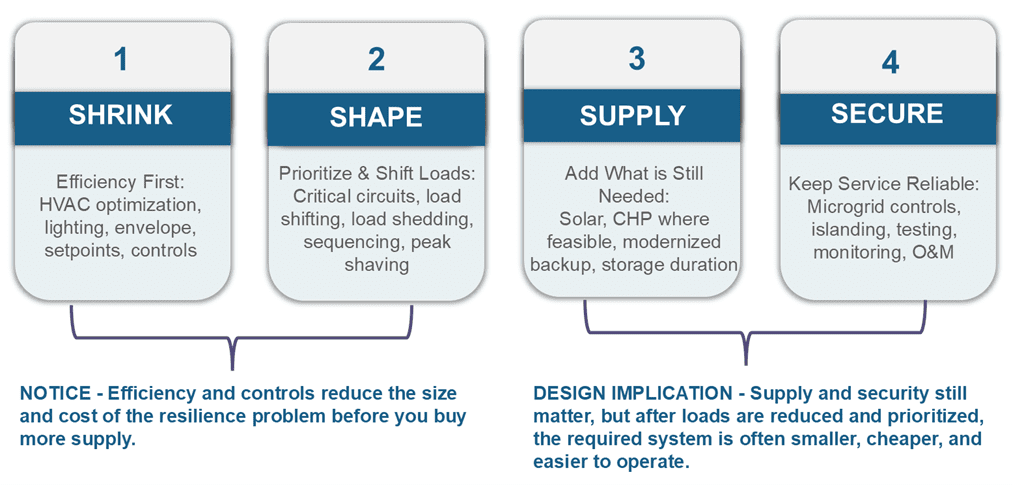
The Four Buckets: Shrink, Shape, Supply, and Secure
EaaS isn’t a single technology; it’s an engineered service built from four buckets
Exhibit G: Efficiency and controls reduce the size (and cost) of the resilience problem. The cheapest resilience is the resilience you don’t need; reduce and prioritize loads before adding supply.
Economics & contracting
Measurement & Verification (M&V): the backbone of fairness
If payments depend on savings, define:
- Baseline period (e.g., 24–36 months)
- Adjustment factors (weather, occupancy, service line changes)
- What counts as savings (kWh, kW demand, fuel, maintenance, avoided rentals)
- Independent verification and audit rights
EPA’s ESPC overview underscores the centrality of guaranteed savings and performance accountability. (EPA, n.d.-b)
Service Level Agreement (SLAs) / uptime guarantees (resilience is a service, so specify it)
For rural healthcare, a serious EaaS contract should define:
- Critical circuits and kW served
- Minimum runtime under defined scenarios
- Response time for faults
- Maintenance/testing schedule
- Penalties or remedies for non-performance
Use FEMA and ASPR TRACIE outage-planning guidance as your “requirements backbone” to translate planning needs into contract specifications. (ASPR, n.d.; FEMA, 2020)
Pricing structures (common)
- Fixed service fee(bundled, predictable)
- Shared savings(provider paid from verified savings)
- Availability payment(pay for guaranteed capacity and uptime)
- Hybrid (often best: efficiency supports resilience economics)
In performance-based models, pricing is structured to align payments with the value delivered. The U.S. EPA notes that energy savings performance contracting is designed to deliver savings “at least equal to the amount of the payments needed to finance the improvement(s),” and may use a “shared savings” approach. Likewise, FERC explains that capacity markets pay not for energy produced, but for “the ability to produce power when needed,” a useful parallel to EaaS contracts that pay for guaranteed uptime and standby capability. (EPA, n.d.-b; FERC, 2025).
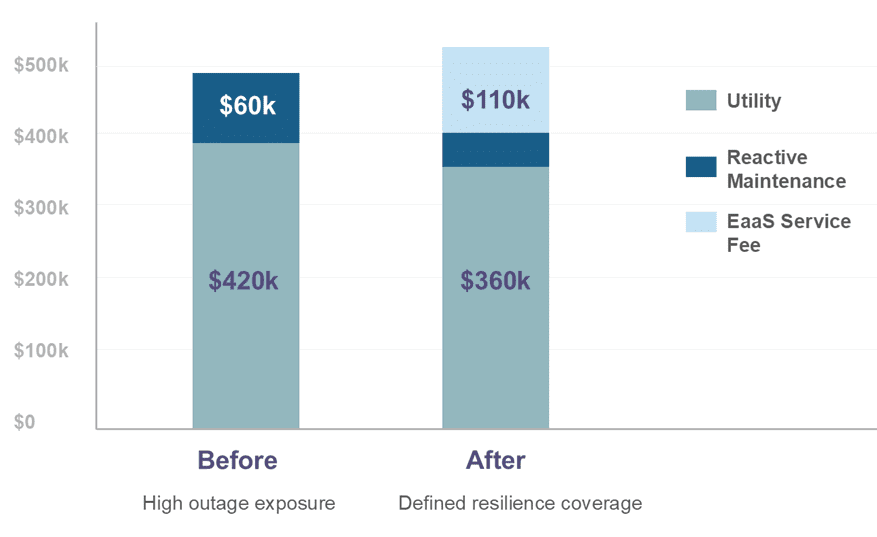
Annual Cost & Outage Risk Exposure
Exhibit H (example scenario): EaaS can reduce utility costs and reactive maintenance while adding a service fee that buys defined resilience outcomes (coverage, uptime, response time). The economic case is often risk-adjusted: fewer emergency rentals, fewer spoiled medications, fewer canceled procedures, and less crisis labor.
Evaluate EaaS in 8 Steps
Move from clinical priorities to technical scope, then to economics, procurement, and governance. That order helps avoid overbuilding and weak contracts.
Exhibit I: A repeatable process that works for a CAH, clinic network, or LTC facility. The first decision is not vendor selection; it’s defining critical loads and acceptable downtime.

How to Evaluate EaaS: Step-by-step decision framework
Step 1 — Define clinical continuity requirements
List critical services and maximum downtime (ED, OR/procedures, refrigeration, IT/telehealth). Use FEMA/ASPR guidance as a starting structure. (ASPR, n.d.; FEMA, 2020)
Step 2 — Quantify your “energy risk exposure”
- Outage history and near-misses
- Generator test results and known vulnerabilities
- Estimated cost of downtime (canceled cases, rentals, spoilage, overtime)
Step 3 — Establish baseline energy performance
Benchmark EUI and identify no-regrets efficiency measures. (EPA, 2015)
Step 4 — Decide your preferred procurement lane
Capex vs EPC/ESPC vs EaaS
Step 5 — Build a scope that starts with load reduction + priority controls
Then add supply (solar/storage/generator modernization) sized to your critical load, not your whole campus.
Step 6 — Demand contract clarity
- M&V rules, baseline adjustments
- SLAs (kW, hours, response times)
- Buyout/termination options
- Interoperability and data ownership
- Insurance and liability
Step 7 — Validate operability
Commissioning plan, drills, training, and a monitoring dashboard your team can actually use.
Step 8 — Make the “risk-adjusted” business case
Include avoided emergency costs and compliance confidence, not just utility bill savings. EIA outage context helps frame why rare events dominate risk. (EIA, 2023)
Funding & complements
Incentives and programs change, verify current eligibility and timing:
- Clean electricity investment credits/energy storage: IRS guidance and updates (track current-year rules and elective pay/transferability as applicable). (U.S. Internal Revenue Service [IRS], 2026)
- USDA Community Facilities: affordable funding for essential community facilities in rural areas (hospitals included). (U.S. Department of Agriculture, Rural Development [USDA], n.d.)
- USDA Rural Energy for American Program (REAP): targeted to agricultural producers and rural small businesses, may apply to certain rural health entities, depending on structure; use the Federal Register Notice of Funding Opportunity (NOFO) for specifics.
- FEMA mitigation programs: availability and structure can change; consult current FEMA guidance and note recent CRS reporting about BRIC developments.
Conclusion & “Next 30 Days” action plan
Next 30 days
- Convene a 60-minute cross-functional meeting (CFO, Facilities, IT, Clinical, Compliance).
- Build a one-page critical load list and downtime tolerance map.
- Pull 24 months of utility bills and any interval data.
- Inventory generators, ATS, switchgear age/condition, and last test outcomes.
- Choose your procurement lane (capex, EPC/ESPC, EaaS) and draft an evaluation rubric.
- Shortlist partners and request concept proposals that include resilience SLAs and M&V plans.
- Identify complementary funding sources and assign someone to verify current eligibility.
Final key takeaway: Rural healthcare can’t afford energy fragility; EaaS is one credible pathway to buy measurable resilience and predictable cost while reducing operational burden, as long as you contract for outcomes and de-risk governance.
References:
American Council for an Energy-Efficient Economy. (2019, February 7). Emerging opportunities: Energy as a service. https://www.aceee.org/topic-brief/eo-energy-as-service
Centers for Medicare & Medicaid Services. (n.d.). Emergency preparedness rule. U.S. Department of Health & Human Services. Retrieved March 18, 2026, from https://www.cms.gov/medicare/health-safety-standards/quality-safety-oversight-emergency-preparedness/emergency-preparedness-rule
Centers for Medicare & Medicaid Services. (2023, March 31). QSO-23-11-LSC: Categorical waiver—Health care microgrid systems (HCMSs). U.S. Department of Health & Human Services. https://www.cms.gov/files/document/qso-23-11-lsc.pdf
Chartis Center for Rural Health. (2024, February 15). Unrelenting pressure pushes rural safety net crisis into uncharted territory. Chartis. https://www.chartis.com/insights/unrelenting-pressure-pushes-rural-safety-net-uncharted-territory
Federal Emergency Management Agency. (2020, July). Healthcare facilities and power outages. U.S. Department of Homeland Security. https://www.fema.gov/sites/default/files/2020-07/healthcare-facilities-and-power-outages.pdf
Federal Energy Regulatory Commission. (2025, April 1). Understanding wholesale capacity markets. https://www.ferc.gov/understanding-wholesale-capacity-markets
National Institute of Standards and Technology. (2023, September). Guide to operational technology (OT) security (Special Publication 800-82 Rev. 3). U.S. Department of Commerce. https://csrc.nist.gov/pubs/sp/800/82/r3/final
National Renewable Energy Laboratory. (2019). Microgrids for energy resilience: A guide to conceptual design and lessons from defense projects (NREL/TP-7A40-72586). U.S. Department of Energy. https://docs.nrel.gov/docs/fy19osti/72586.pdf
U.S. Department of Agriculture, Rural Development. (n.d.). Community facilities direct loan & grant program. Retrieved March 18, 2026, from https://www.rd.usda.gov/programs-services/community-facilities/community-facilities-direct-loan-grant-program
U.S. Department of Energy. (n.d.-a). Energy service agreements (ESAs). Better Buildings Solution Center. Retrieved March 18, 2026, from https://betterbuildingssolutioncenter.energy.gov/sites/default/files/news/attachments/RILA%20ESA%20Primer.pdf
U.S. Department of Energy. (n.d.-b). Healthcare. Better Buildings Solution Center. Retrieved March 18, 2026, from https://betterbuildingssolutioncenter.energy.gov/sectors/healthcare
U.S. Department of Energy. (n.d.-c). Cybersecurity baselines for electric distribution systems and distributed energy resources (DER) and guidance. Office of Cybersecurity, Energy Security, and
Emergency Response. Retrieved March 18, 2026, from https://www.energy.gov/ceser/cybersecurity-baselines-electric-distribution-systems-and-der-and-guidance
U.S. Department of Health & Human Services, Office of the Assistant Secretary for Preparedness and Response. (n.d.). Planning for power outages: A guide for hospitals and healthcare facilities. ASPR TRACIE. Retrieved March 18, 2026, from https://asprtracie.hhs.gov/technical-resources/resource/4033/planning-for-power-outages-a-guide-for-hospitals-and-healthcare-facilities
U.S. Department of Health & Human Services, Office of the Assistant Secretary for Preparedness and Response. (2019, February 26). CMS emergency preparedness rule generator requirements (ASPR TRACIE technical assistance). https://files.asprtracie.hhs.gov/documents/aspr-tracie-ta-cms-ep-rule-generator-requirements-2-26-19.pdf
U.S. Energy Information Administration. (2023, October 2). U.S. electricity customers averaged five and one-half hours of power interruptions in 2022. Today in Energy. https://www.eia.gov/todayinenergy/detail.php?id=61303
U.S. Energy Information Administration. (n.d.). Reliability metrics (SAIDI and SAIFI). Electric Power Annual. Retrieved March 18, 2026, from https://www.eia.gov/electricity/annual/html/epa_11_03.html
U.S. Environmental Protection Agency. (2015, January 29). Energy use in hospitals (DataTrends). ENERGY STAR. https://www.energystar.gov/sites/default/files/tools/DataTrends_Hospital_20150129.pdf
U.S. Environmental Protection Agency. (n.d.-a). Learn about impacts of diesel exhaust and the Diesel Emissions Reduction Act (DERA). Retrieved March 18, 2026, from https://www.epa.gov/dera/learn-about-impacts-diesel-exhaust-and-diesel-emissions-reduction-act
U.S. Environmental Protection Agency. (n.d.-b). Performance contracting and energy service agreements. Retrieved March 18, 2026, from https://www.epa.gov/statelocalenergy/performance-contracting-and-energy-service-agreements
U.S. Government Accountability Office. (2020, December 22). Rural hospital closures: Affected residents had reduced access to health care services (GAO-21-93). https://www.gao.gov/products/gao-21-93
U.S. Internal Revenue Service. (2026, January 5). Clean electricity investment credit. https://www.irs.gov/credits-deductions/clean-electricity-investment-credit






